FOR PATIENTS, HOSPITALS, AND CAREGIVERS
Care Continuity
Patient Controlled
No Staff Burden
Introduced at Discharge
Outcome Data
Safety Plan
Patient Controlled
Give patients and family agency, connection and support after discharge beyond a paper treatment plan and a hotline.
- Participant-controlled
- No IT systems required
- No PHI or EMR integration
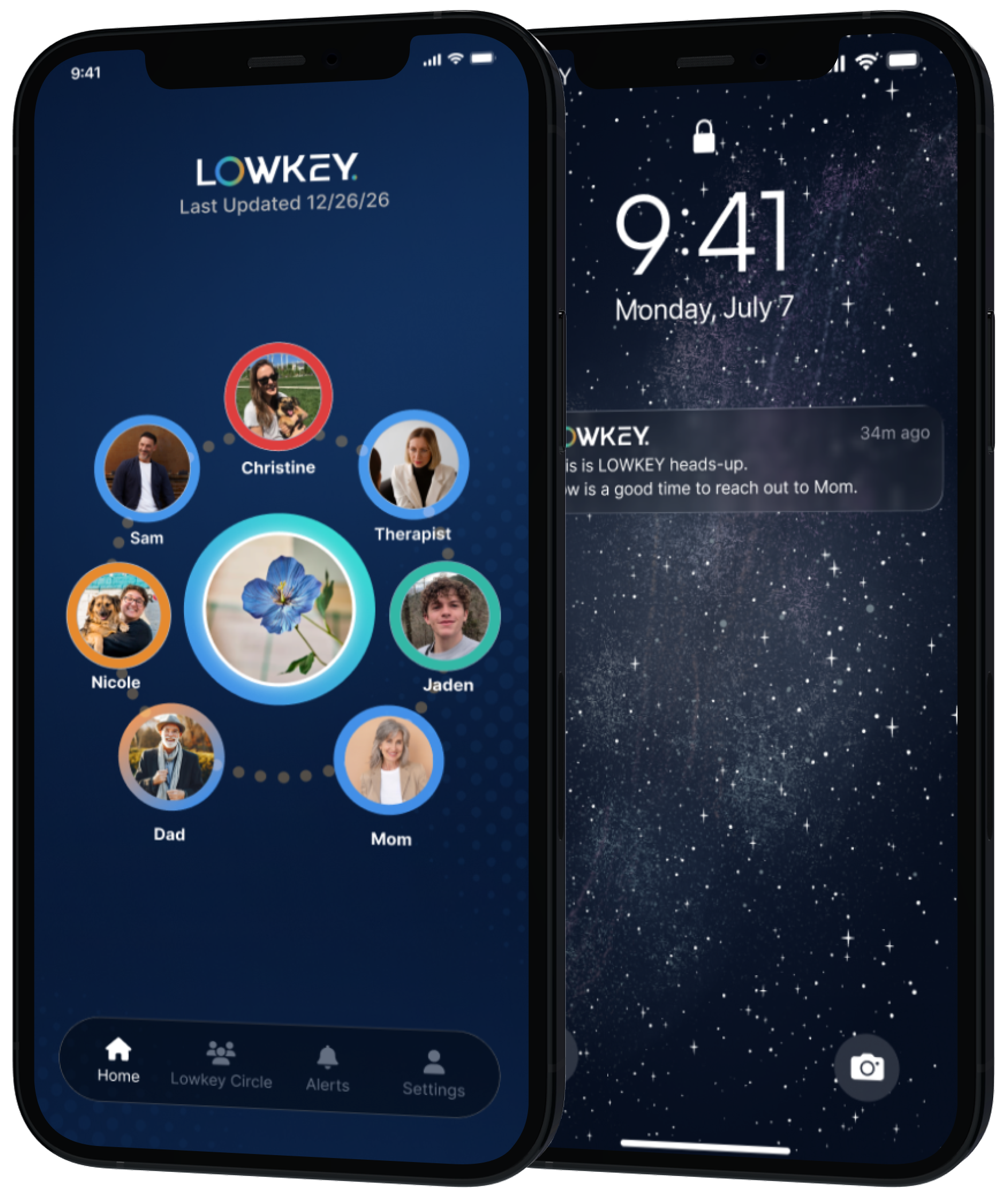
When Support Ends, Uncertainty Begins
- Inpatient therapists focus on active patients not alumni
- Alumni programs are asked to demonstrate continuity outcomes using surveys.
- Families don’t know when to step in
- Insurance companies demand post-discharge outcomes without providing infrastructure
The window between stable and crisis is where outcomes are won or lost.
There’s a Better Way
How LOWKEY Works
Seamless integration into your discharge process with zero technical overhead.
Introduced at Discharge
Takes less than 5 minutes during exit planning.
Participant installs app
They choose their circle (peers, family, therapists—by invitation only).
Learns baseline behavior
Baseline learning period (7 to 21 days) to establish personal patterns.
Alerts on sustained deviation
First to the participant. Then to their chosen support circle, if needed.

“My family knows what it is like to live in the gap between ‘Are you ok?’ and 911. People deserve something better, so we created a technology and relationship infrastructure that works proactively for the participant, independently of the system.”
— Jennifer Cunningham, Founder and CEO
Benefits
A Thermometer for Daily Life™ Not a Surveillance System
LOWKEY was built on one principle: preserve patient autonomy while extending continuity of care.
Early awareness
Just signals, no diagnosis
Proactive information
No manual logging required.
Timely Connection
Chosen relationships with a prompt to connect
Built in Collaboration with Treatment Professionals & Alumni
“LOWKEY is much more authentic and empirical than what is being gathered today. Now we can have data on behavioral trends – not just how somebody feels and not through surveys.”
— James Meyer, Treatment Center Consultant, Adolescent Programs
Why Centers Use LOWKEY
Treatment centers need proof of outcomes without increasing staff burden or costs.
Improve Contracts for Safety
Payers and accreditation bodies want evidence of post-discharge support. Lowkey gives you something documented, consent-based, and concrete to show them.
Fewer Readmissions and Cost Savings
A readmission costs you a bed, a staff team, and a payer relationship. Lowkey catches the decline before it becomes one.
Market Differentiation
Most centers look identical at discharge. Lowkey gives you something competitors can’t claim: care that continues after the patient leaves your building.
Post-Discharge Data
You know who came back. You don’t know what the 90 days before looked like. Lowkey closes that gap without dashboards or clinical review.
Avoid Future Penalties
Centers that can demonstrate reduced readmission rates will have the evidence to fight penalties, negotiate better insurance contracts, and attract referrals.
Better Adherence
Patients connected to people they trust are less likely to isolate. Lowkey keeps that connection active after discharge, without touching your team’s workload.

Why Alumni Choose LOWKEY
After treatment people are ready to begin again. LOWKEY provides independence with connection and support without supervision.
Autonomy
You control who's in your circle and what they see. No oversight, no reporting — just people who care.
Proactive Insights
Passive, early signals trigger self check-ins—no manual logging required.
Continued Support
Discharge with a tool designed to support self, not just report on you.
Trusted Bonds
Preserve the meaningful bonds created in treatment with your chosen circle.
Continuity of Care
Helps fill the gap between 'are you ok?' and a crisis event.
Financial Safety Net
Insurance to protect against $15K–$40K readmissions or $3k emergency visits.
Designed for Your Entire Organization
Clinical Directors
Proof of outcomes without added clinical burden. Objective data to support value-based care negotiations.
Alumni Coordinators
Tools to foster genuine connection, not just attendance tracking. Scalable engagement for growing alumni pools.
CEOs & Executives
Differentiate your program, strengthen payer relationships, and unlock potential reimbursement revenue streams.
Family Directors
Provide families with peace of mind and a safety net without creating codependency or intrusion.
Try it. See if it Fits.
Your Role:
- Introduce LOWKEY at discharge
- Decide pricing model (included or pass-through)
- Encourage peer invitations
Cost
Staff
Pilot Details
- Duration
- Participants
- Cost
- Pricing
- 60 days
- 25–50
- $0
- $14.99/mo per participant
See if LOWKEY. fits your program
Data, Privacy & Compliance
Participant Controlled
LOWKEY is client-facing. Programs receive no patient-level data. Notifications go only to the support circle.
Private by Default
No location tracking. No EMR integration. No PHI collected. No identifiable data sold.
Secure Infrastructure
SOC 2–compliant hosting. End-to-end encryption. On-device GPS processing only.
Built for Industry Standards
Apple HealthKit data.
Uses passive behavioral data from iPhone and Apple Watch.
Supports CARF Continuity of Care
- Maintains connection after discharge
- Enables objective continuity measurement
- Supports person-centered care
- No staff burden or monitoring
The Transformation
Real World Impact
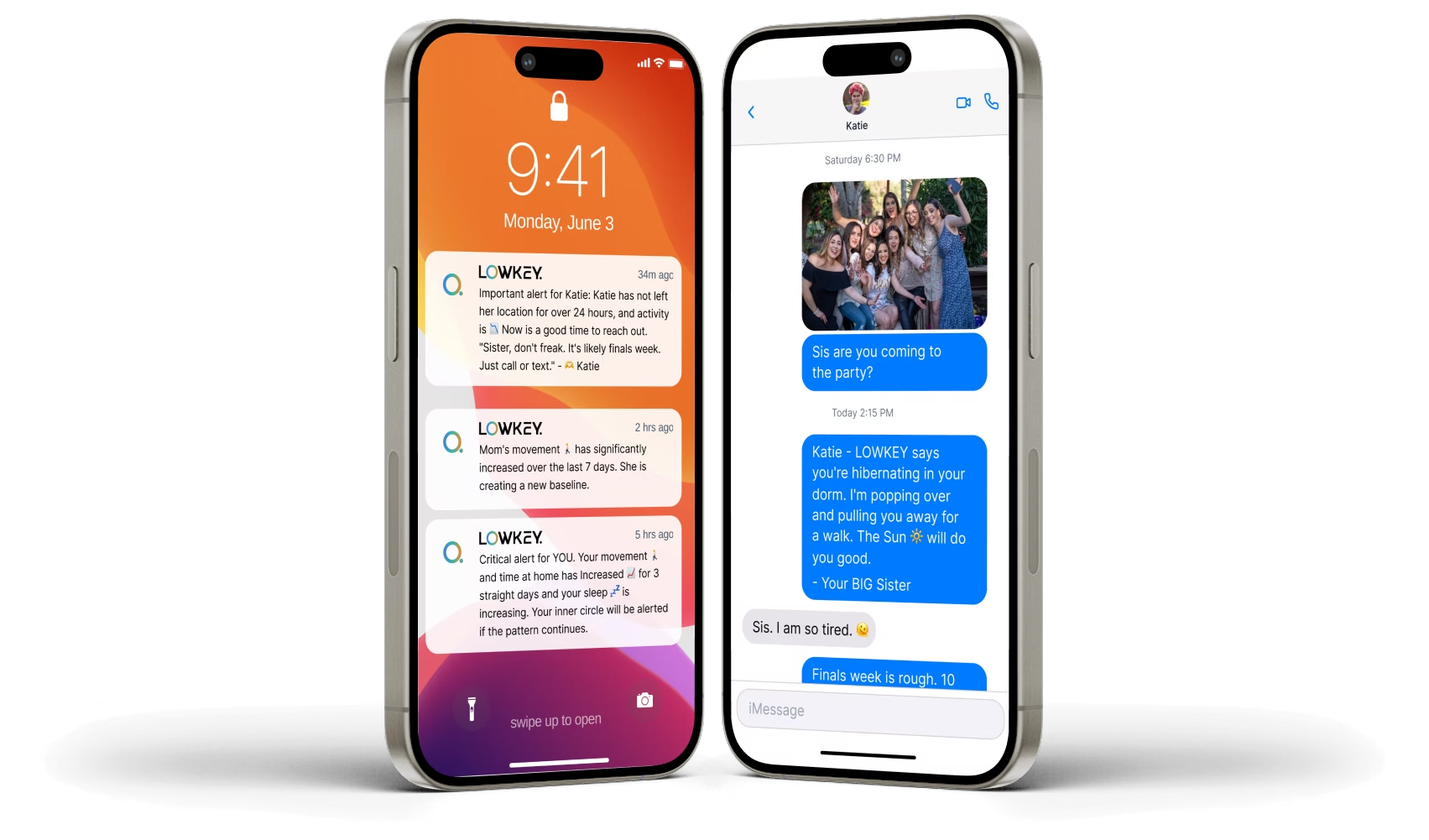
“A 22-year-old leaves your program. Day 18, her sleep drops 40% and she stops leaving the apartment. Her peer from treatment gets an alert and calls. She re-engages with her therapist.”
Built by People Who Understand the Gap
Combining deep clinical expertise, consumer technology scale, and military-grade security.

Nathaan Demers, Psy.D
Advisor — Clinical Psychology

Jud Valeski
Advisor — Engineering & Product

Jennifer Cunningham
Founder & CEO

Eric Reid
Advisor — Engineering & Product

Dennis Bach, RN
Advisor
Frequently Asked Questions
Is LOWKEY a medical or crisis tool?
No. LOWKEY is a wellness trend-tracking tool. It does not provide medical advice, diagnosis, or emergency intervention. If you or someone you know is in crisis, contact emergency services or call/text 988.
How does LOWKEY fit alongside our clinical care?
LOWKEY is participant-controlled and runs outside clinical workflows. It is not a clinical, diagnostic, or crisis-response tool.
What about HIPAA and privacy?
LOWKEY is not designed to collect protected health information. It does not collect diagnoses, treatment records, or clinical data. LOWKEY uses limited, non-identifiable daily pattern signals (such as sleep consistency and general activity trends) to generate non-clinical notifications. It is not a medical record and does not integrate with the EHR.
Do treatment centers receive notifications?
No. All notifications go to the participant and the people they choose to include. Program involvement is always optional and always initiated by the individual.
Does this require staff training or workflow changes?
Introduce LOWKEY as an optional resource during discharge. That is the extent of staff involvement. There are no dashboards to check, no notifications to respond to, and no ongoing operational responsibilities. LOWKEY operates between the individual and the people they choose to include.
How does LOWKEY fit with existing discharge or aftercare workflows?
It doesn’t change them. LOWKEY is introduced as an optional continuity resource during discharge planning. After setup, it runs independently and does not require documentation, monitoring, or ongoing involvement from staff.